How We Finally Won the Battle Against Eczema

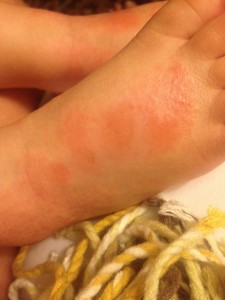
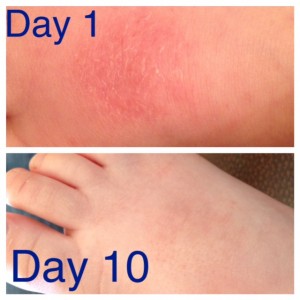
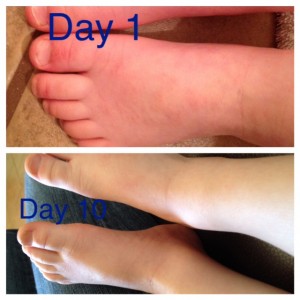
November 2013 – the tops of his feet became our hot spots that never really cleared. You can see the skin was raw and oozing here.
Many of you already know the numerous things we as parents will try to find, eliminate or treat our kid’s eczema triggers. I am part of a wonderful community of parents who offered advice on how to heal the skin naturally including essential oils, coconut oil, goat soap, elimination diets, detergents, probiotics, changing bath soaps, and all the best lotions. I appreciated every suggestion and sample thrown our way.
I hated the thought of using steroids on my infant and agreed that masking the symptoms of eczema was not the best way to solve our problems. We needed to find the problem causing the eczema. Callen was diagnosed with eczema at his 2 month appointment prior to receiving any vaccinations. I know some people question that. He was also exclusively breastfed. He had some red splotches on his belly and back that had been there a couple of weeks so I think it started around 6 weeks. Callen turned 1 in July 2013 and two months later we had our first blood tests with these results. Results: Moderate IGE for Eggs (.75) & Peanuts (3.28) and Low for Sesame Seed (.45)
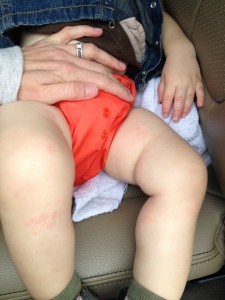
During this flare, spots spread further up his legs and on his face. His diaper area was the worst. He had never had diaper rash before so I was struggling to figure out if we were dealing with typical diaper rash or if the eczema was taking over.
The next step was to see a dermatologist who prescribed the same steroids our pediatrician had us on except she directed us to use them more often. She didn’t believe in a link between food allergies and eczema. I came away from that appointment feeling disheartened that we were left to keep medicating without finding a reason for all the problems our little boy was having. Soon after, we had our first appointment with a highly recommended allergist for our first skin test. The appointment lasted over 4 hours. I hugged my son as they administered all the tiny pricks into his back with my husband behind me to hold my son’s arms. They both had tears. It was pretty hard.
The results of the skin test confirmed a suspected peanut allergy (35 IGE). Callen had a Reese’s cup at Halloween 4 ½ months earlier and he vomited 20-30 minutes after. He was 16 months old. We assumed he got sick from something else that day but I knew vomiting was a sign of food allergy. We knew peanut was on the blood test but I had read about false positives and didn’t know for certain how much a food would really affect him. I guess he had to have had peanut sometime prior to Halloween in order for his body to show the reaction it did to the test but Halloween was the first time I know of and the first time he’d ever vomited.

Results: Peanut and Avocado were high with several other things like walnut, almond, horse, dust mites, dog dander and pollens from pecan, cedar, cottonwood, oak and Bermuda getting ranks too.
We assumed we were still missing a food allergy or other trigger. I got an app on my phone to help me track his skin and the allergy forecasts for that day to try to link something. We returned to the allergist for more skin testing. This time my husband and I traded places with him hugging my son and I held his arms. I was in tears this time around.
SKIN TEST RESULTS***
After this test, we removed even more food from Callen’s diet. Beef, chicken, and his favorite breakfast, oatmeal. We also assumed the creek and trees behind our house must be harboring one of the molds he had such a high reaction to. The eczema had always been a part of our lives but it was really starting to affect the whole family’s sleep. During the summer of 2014, we pulled out all the stops. Our last ditch efforts included removing what little carpet we had in our house which was only in the bedrooms. I took my son to my grandma’s house for a weekend while my husband laid laminate flooring so that my son was not even around when things got stirred up. We also sent our dog to live with my parents. I had her before I even started dating my husband! I spent over $100 on a chiropractor who didn’t accept insurance in the hopes he would have something new to offer. I purchased dust mite casing for our bedding which was $150.
We explored the idea that maybe eczema wasn’t the whole story. We were homebound, unable to drive anywhere because he’d remove his shoes and socks and start scratching while I was driving. Our neighbor drove us to the lab for more blood work to test Vitamin D and Zinc levels which both came back normal. I was far into my 2nd pregnancy and restraining my son as they drew blood. I couldn’t help but sob. The poor tech probably had no idea how to respond to a desperate pregnant woman with a miserable toddler.
We were using wet wraps for 2 weeks and steroids and I saw no improvement. I decided to stop using them. I had a new Rx for Protopic…well, it wasn’t new. I’d had it for a while but had delayed trying it because it is an immunosuppressant. I used Protopic at the same time I stopped steroids. I didn’t realize it at the time but that was the absolute wrong way to go about it! Callen’s whole body flared up like never before.
I was on Facebook and found a group for TSW or Topical Steroid Withdrawal. I decided to give it a try and see if Callen could pull out of this vicious cycle on his own through persistence and really narrowing down his diet. Even the parts of his body that weren’t red felt like a reptile. This TSW period lasted about 2 months (August – September 2014) and it was the most depressing and tormenting time in our lives. He was eating only turkey and fruits and veggies. We removed the known allergies plus more including dairy, nightshades and citrus just to be extra cautious. And no sweets. His skin continued to deteriorate. I could not stop the tears from flowing. I was falling into some depressive thoughts feeling hopeless. I wondered how on earth my son would survive in life if his body’s largest organ, the skin, wasn’t functioning properly to protect him from his environment. We were running on very little sleep night after night for months. I started having visions of a funeral. I sobbed and sobbed and prayed and prayed. I quit my contract job earlier than planned to be his caregiver full-time. I told my boss there was no way around it. My son needed me more. Eczema was fully controlling every minute of our lives.

Meal times were awful. We could hardly leave him alone in the high chair. His feet would be “scissoring” or “cricketing” as we called it. And here he is scratching with his fork.
During our “Topical Steroid Withdrawal” period, we contacted National Jewish Health in Denver, CO and got scheduled for a 2-week outpatient program starting roughly 2 weeks after our daughter was born. This was tricky to plan seeing how we didn’t know exactly when she’d be born and decided flying my husband and son would be the best option so that Callen wouldn’t be subjected to such a long road trip while fighting the itch seeing how we couldn’t even drive 5 miles from home. I recruited a friend to help me make the drive in order to keep our newborn out of the airports and other public spaces. This was my first night away from Callen and I worried out of my mind how Phil could manage a night on his own. Once Ada was born, she and I slept in another room so her waking wouldn’t set Callen off. Phil would text me to come help him in our room to apply more cream or just to go to the bathroom. I knew NJH would use steroids so the two nights prior to their flight, Phil used them and got by. Our trip to NJH was a lifesaver in helping us get a grasp on his skin. We started with an intensive program of soak and seal also known as wet wrapping. I was floored when my husband, Phil, sent me a picture of our son wrapped from head to toe while I was away getting us checked out of our hotel so we could move into the Ronald McDonald House. Callen’s skin started healing and they conducted more skin tests.
I was so glad to see different results and watch Callen pass the oral food challenges! This meant we could regain some normalcy in our lives like eating out. We were educated on sleep cycles and also found out that Callen had low iron which correlate with troubled sleep. We left NJH with a sense of cautious confidence. I cried tears of appreciation when we left. The NJH program costs around $17K. Thankfully, insurance covered most of it and our dear friends and family rallied with a Go Fund Me account which helped cover our portion. This relieved a lot of stress so that we could just focus on getting the training we needed to help our little guy heal. We returned home with a plan. We did two baths a day which required almost an hour each counting getting him fully creamed and dressed after a minimum soak of 20 minutes. This included medicated shampoo in the mornings and steroid on his scalp for the night bath. We also did nasal rinses which felt like waterboarding. He took Zyrtec and iron in his OJ every morning and Singulair and Atarax/Hydroxizine with melatonin every night. It doesn’t sound like a lot but it was pretty rigorous.

This was our set up of ointments and layers of clothing after each bath. This continued for 4 months post-NJH at home while I cared for a newborn at the same time and we did this twice a day everyday.
The proper way to get off of steroids is to taper off very slowly. NJH explained how to do this but I was really struggling to step down to anything less than daily applications which discouraged me. Just before we went to Denver, I started following a FB page for Dr. Aron. I decided it was time to register for Dr. Aron’s treatment. I was getting burnt out doing 2 baths/day after 5 months. If there was a better way, I wanted to check it out. Our first batch of cream was mixed by me at home. I thought I did a thorough job but after a conversation with a fellow dad in MO, decided I should give the professional compounders a shot because I wasn’t seeing results after about 2 weeks. Phil was asking to return to our previous steroid. I needed to know we were giving it a fair shot before we gave up. I picked up the new batch on Thur, Jan 29, 2015. I applied it once that evening but noticed the consistency wasn’t what I expected. The pharmacy didn’t get the mix exactly right. They used ointment for one of the components rather than cream. This isn’t what Dr. Aron prefers but our local pharmacies wouldn’t have a compounder in again until the following Monday so we used what we had.
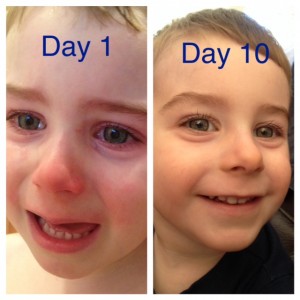
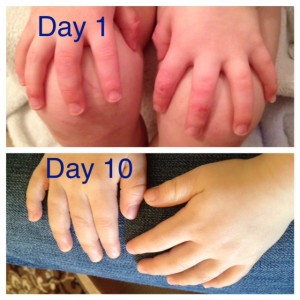
Callen slept great that night. Was it a fluke? Was it because he’d had a cough and maybe he was just super tired from being sick? The next night Callen didn’t want to wear socks. Socks and full 100% cotton pajamas have been mandatory to help protect his skin. We decided it was fine and that if he started itching later, we’d put socks on then. Another night of great sleep. He was only waking at night during coughing fits. The next night he chose shorts to sleep in and we obliged thinking maybe it keeps him cooler at night. A full week later, and he slept great every single night! I weaned him off the small dose of melatonin he’d been getting during the first week and Atarax the second week. He’s taken that nightly since before our Denver trip in October…probably since August. We have 2 months behind us and are currently tapering successfully!
We are 7 months into treatment and with summer being a hard season for us, we increased to two apps/day but only on a handful of very tiny places like two mid-fingers, two toes and the occasional place by his eye or under his nose. Outside of that, no additional lotions, creams or ointments!
So, if your child is showing allergies to every food they eat, don’t settle that that is permanent. If you are struggling to decrease steroid use, consider the power of diluting like Dr Aron does along with antibiotic to attack the staph. If you are making crazy Excel charts to help you remember where you last put which medicine, choose Aron Regime. It’s affordable and also the most simple and incredibly effective!
Just a quick update as of July 2016 – Callen’s feet had some issues by the end of June. Typical season for him. With a little medication under cling wrap on the bottom of his toes, his feet were healing up after a week. Too bad we waited a couple weeks thinking it was athlete’s foot. He’s back on track and we apply our Aron cream 1-2 x/daily on his feet and occasionally on his scalp. We are now 18 mo into treatment and still doing fabulous. Callen is growing well, eating well and has even started a food allergy treatment called Oral Immunotherapy that would not have been an option if his eczema was still out of control.